Today’s guest post is written by Ijeoma Kola, a PhD candidate in Sociomedical Sciences at Columbia University Mailman School of Public Health and a former National Science Foundation graduate fellow. Her dissertation examines the history of asthma in urban African Americans in the 20th century, with special attention to medical history, environmental racism, and community activism. On Tuesday, November 14 at 6pm, Ijeoma will give the talk “Unable to Breathe: Race, Asthma, and the Environment in Civil Rights Era New Orleans and New York.” Click HERE to register for this event.
In July 1965, several months after the assassination of Malcolm X and the freedom marches from Selma to Montgomery, the New York Times ran a story about “an emotional epidemic” of asthma sweeping across New York City.[1] Although the writer focused on psychosomatic explanations to link asthma symptoms to the hostility of the Civil Rights Movement, it prompted me to explore the significance of asthma’s emergence as a racial problem during the 1960s.

Osmundsen, John A. “Asthma Linked to Rights Drive.” New York Times. 1965.
Before the 1960s, little was written about asthma in African Americans. For much of the early twentieth century, doctors debated whether black people could have asthma, as they understood the disease to afflict middle and upper-class whites, who were believed to have more civilized lifestyles and delicate constitutions than poor blacks.[2]
However, in the 1960s, several “outbreaks” of asthma made national news headlines. In the fall of 1960, nearly 150 patients from adjoining neighborhoods were treated for asthma at Charity Hospital in New Orleans. One patient, a 73-year-old man, died.[3] After several years of seasonal asthma admission spikes in the same hospital, researchers at Tulane University found that asthma related visits to the emergency room correlated with fire department calls from spontaneous fires at the base of garbage heaps, some five to twenty years old, around the city. Smoke containing silica particles would drift downwind to where the majority of people who visited Charity Hospital, triggering asthma attacks.[4]
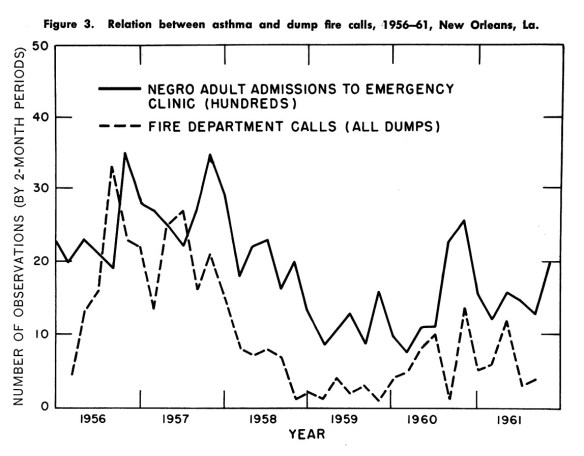
Lewis, Robert, Murray M. Gilkeson, and Roy O. McCaldin. “Air Pollution and New Orleans Asthma.” Public Health Reports 77, no. 11 (November 1962): 953.
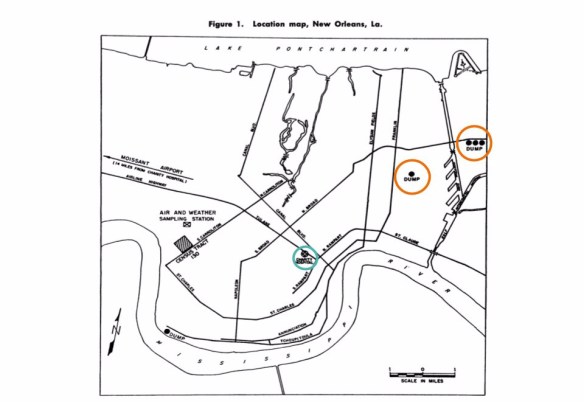
Lewis, Robert, Murray M. Gilkeson, and Roy O. McCaldin. “Air Pollution and New Orleans Asthma.” Public Health Reports 77, no. 11 (November 1962): 948. with modifications.
At the time, however, the New Orleans asthma epidemic of November 1960 was quickly forgotten, as events over the course of the next few days would quickly turn attention away from asthma to something more urgent. A week after Dennis Knight’s death, on November 14, 1960 – four black 6-year old girls – Leona Tate, Tessie Provost, Gaile Etienne, and Ruby Bridges – began the school integration process at two elementary schools in New Orleans. Violent protests broke out across the city, and only 13 of the usual 1,000 students at the two schools attended on integration day.[5]
In New Orleans in 1960, and in several other American cities with a large concentrated black community over the next decade, asthma appeared to present itself alongside moments of racial tension. Although the New York Times connects these two phenomena with a psychosomatic explanation of emotional distress, I view the relationship differently. Neighborhoods where African Americans lived – often restricted to due to segregation and redlining – were more exposed to both indoor and outdoor particles that triggered asthma symptoms. While struggling to breathe, black people simultaneously fought for the right to live as equals. Rather than think of Civil Rights as a cause of asthma, I see asthma outbreaks in black urban America and subsequent efforts to reduce the asthma disparity as both a symptom and a symbol of the Civil Rights movement.
References:
[1] John A. Osmundsen, “Asthma Linked to Rights Drive: Authorities Note Sharp Rise in Ailment Among Negroes and Puerto Ricans in City CAUSE STILL UNCERTAIN Tensions of Fight for Gains Play at Least Some Role, Many Experts Contend,” New York Times, 1965.
[2] Horace F. Ivins, “Pollen Catarrh-Hay Fever,” in Proceedings of the Fourth Quinquennial Session of the International Homoeopathic Congress, Held at Atlantic City, N.J., U.S.A., June 16 to 22, 1891 (Philadelphia: Sherman & Co., 1891), 732–43.
[3] “Medics Puzzled:: Asthma Epidemic Hits New Orleans; 149 Seized, 1 Dead,” Philadelphia Tribune (1912-2001); Philadelphia, Penn., November 12, 1960, sec. 2.
[4] Robert Lewis, Murray M. Gilkeson, and Roy O. McCaldin, “Air Pollution and New Orleans Asthma,” Public Health Reports 77, no. 11 (November 1962): 947–54.
[5] John G. Warner, “Mob of 5000 Is Hosed By New Orleans Police: Police Hose New Orleans Segregation Rioters,” The Washington Post, Times Herald (1959-1973); Washington, D.C., November 17, 1960.

