Today we have part two of a guest post written by Dr. Daniel S. Goldberg, 2016 recipient of the Audrey and William H. Helfand Fellowship in the History of Medicine and Public Health. Part one can be read here.
X-ray exhibitions were hugely popular all over the country, and the greater NY area was no exception. At a February 1896 demonstration run by Professor Arthur Wright, director of the Sloan Laboratory at Yale University, a newspaper reported that despite the auditorium being literally jam-packed, students were still crawling through windows 30 minutes into the lecture — and all this despite the fact that none of the audience, save those in the first few rows, could even hear Wright’s discussion. The deans of multiple Yale schools (Divinity, Law, and Science), the head of the Yale Corporation, and the chief medical examiner were all in attendance.
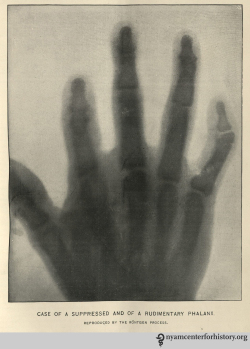
Perhaps the first published X-ray in the United States of a clinical condition. In “Rare Anomalies of the Phalanges Shown by the Röntgen Process,” Boston Medical and Surgical Journal 134(8), February 20, 1896: 198–99.
The pressing question is “why”? Why did X-rays exert such tremendous power across a wide spectrum of social domains? (X-rays were a constant topic of conversation in sermons and religious journals, in women’s journals, in influential satirical periodicals like Punch, and were the subject of a seemingly endless number of political and non-political cartoons, to name but a few). Although historians of the X-ray have offered a number of plausible answers, I believe there is a key element left unexplored in the historiography: the intellectual frameworks, or ideas, relating to changing ideas of truth, doubt, and objectivity in U.S. society at the time.
Two of these frameworks are most useful in unpacking the stunning impact of the X-ray: the rise of mechanical objectivity, and what can be called “somaticism” within medicine and science. Historians of science Lorraine Daston and Peter Galison explain that a new model of ‘objectivity’ begins to take hold during the middle decades of the 19th century. Under this new model, the truth-value of scientific knowledge is a function of the investigator’s ability to remove or eliminate human, subjective influence from the knowledge-making process. The fact that this is more or less impossible, and that X-rays can be manipulated in all sorts of ways was well-known to contemporaries and remained a source of anxiety for some time. The important point is the ultimate goal: to let the mechanical processes of nature speak for themselves and reveal their truths. Ideas of objectivity, as Daston and Galison point out, have for over four hundred years been connected to scientific images, which makes media like photography and X-rays especially significant.
By the end of the 19th century, ideas of mechanical objectivity begin to fundamentally reshape ideas of what is known and what is certain. This is especially crucial in a century that features so much intense change, including but not limited to governments, family and labor structures, migration patterns, and, of course, industrialization and urbanization. Late Victorians were beset with anxieties connected to their changing world, and they were especially concerned with artifice and deception — that the world was not what it seemed. As such, intellectual frameworks that shaped the criteria for truth were hugely influential, and traveled well beyond narrow networks of scientists and medical men.
Somaticism integrates in important ways with constructs of mechanical objectivity. Historians of medicine have documented the influence of somaticism (or, “empiricism,” as it is also sometimes termed) within medicine over the long 19th century. The core of the framework is that truths about disease and the body are to be found in pathological anatomical objects. The existence of these objects can then be clinically correlated with the illness complaints the patient has, or more likely had given that pathological objects are most likely to be located precisely during a postmortem — until the X-ray. The truths of the sick body are to be found in the natural objects of disease, which makes seeing those objects so essential. Laennec himself explained that the point of the stethoscope was not to listen; listening was merely a means to an end. The point, as Jacalyn Duffin explains, was “to see with a better eye.”
Collectively, these frameworks go a significant length in explaining the enormous and enduring social impact of the X-ray.

Article from the New York Record. May 1896.
For example, Morton’s clippings contain a May 1896 article from the New York Record entitled “X Rays for a Consideration: Light in a Human Kidney.” The article details what may be the first private X-ray laboratory opened in New York City, founded by Mrs. M.F. Martin, and located at 110 East 26th Street. The lab was intended solely for the use of physicians and hospitals. One of its first patients was a doctor named George McLane, who traveled from North Dakota to have his kidney X-rayed for evidence of a possible stone. A surgeon removed McLane’s kidney, and Morton placed it on a plate and subsequently irradiated it with X-rays. The procedure “revealed the absence of any stone in the organ, demonstrating the entire reliability of doctors to prove the absence of stone in the kidney.”
The X-ray shines its light into the hitherto dark spaces inside the human body, revealing the truth of a disputed question: whether McLane suffered from a kidney stone or not. The truth resides in the natural object itself, and the mechanism of the X-ray supposedly insulates the production of medical knowledge from the whims and artifices of the investigator (as compared to illustrations and drawings, for example).
Or, as Dr. McLane himself stated at the Post Graduate Hospital (the primary hospital at which Morton cared for inpatients):
“Dr. McLane spoke modestly at the Post Graduate Hospital about the risk he had taken in the name of science . . . ‘Hitherto a great many mistakes have been made owing to the inability of doctors to prove the absence of stone in the kidney . . .’ Now, by a very simple process, the truth can easily be determined.”
It is difficult to imagine how powerful it must have been, in 1896, to witness an X-ray operator remotely anatomize the living body. Seeing inside the body had been a dream of physicians for centuries prior, and there is every reason to believe that its achievement has not eroded much of its social power. Americans still perform significantly more medical imaging procedures than virtually any of our comparator societies, and what is most interesting is the evidence that this utilization is driven both by supply and demand. That is, it is not merely that we have expensive X-ray and medical imaging machines — so we use them. Across a wide variety of illness paradigms, illness sufferers and patients request medical imaging; they want it to be performed on their bodies. The history of the X-ray helps us understand the enduring power of these tools, of what it means to delve into the penetralium.














 Today’s guest post is written by Harriet Washington, a science writer, editor and ethicist. She is the author of several books, including
Today’s guest post is written by Harriet Washington, a science writer, editor and ethicist. She is the author of several books, including 


















